Is Your Hospital Really Paperless?
As seen in Healthcare IT News.
As seen in Healthcare IT News.
It is tempting to believe that your hospital is now paperless once you’ve implemented an electronic medical record (EMR) system or completed an EHR conversion. While EHRs are the biggest step toward going paperless, most organizations still manage volumes of paper which prevents the establishment of a truly integrated care team – one in which all information is available to all providers in near real time. Organizations that are not completely paperless cannot meet HIMSS Stage 7: a full digital environment where all clinical documents are available electronically within 24 hours of creation or receipt. Documents such as outside records, telemetry strips, ancillary results, signed consents, and “shadow charts” that are part of a patient’s overall record often remain on paper, and leave healthcare organizations with paper to manage and a disjointed care environment. The good news is that going paperless can be achieved in a variety of patient care settings and with minimal disruption.
Eventually it will be possible for patients, healthcare staff and clinicians to enter all data into a patient’s EHR and little or no paper will be required. Until then, improved workflows and exciting new technology can support going virtually paperless. Interested? Then keep in mind a few facts, and don’t let them go as you consider implementing at your facility:
-
With the right technology, scanning can take LESS time than filing to a paper chart
-
Scanning is a form of clinical documentation, it is NOT an “administrative task”
Paperless Is Possible
At Freed Associates, we’ve worked with several healthcare organizations, both large (400 beds) and small (30 beds), to implement a decentralized Point of Service (POS) scanning model to create paperless systems that are improving quality of care, safety and performance. This POS model required the real time scanning of thousands of pages in clinical and registration settings. It eliminated virtually all paper, and expedited the creation of a single and complete EHR. Physicians and care providers no longer have to wonder where documents are or when they will be viewable in the chart.
The right planning and consideration of several key factors will help your facility assess how to roll out the right model for your teams and their patients:
The Benefits of a Decentralized POS Scanning Model
The primary advantage of a POS model is that clinical documentation is in the chart sooner because it is scanned where and when it is created. Additionally, it can be staffing neutral, and can sometimes allow for more resources geared toward clinical care than on administrative tasks. In contrast, centralized models delay chart completion and the initiation of the Revenue Cycle process because they require the documents to be transported and scanned later, often upon discharge. While POS models create a learning curve for the staff that will do the scanning, this is generally normalized within a few weeks of launch.
Our experience indicates that the POS model takes the same or less time to scan as it takes to file to a paper chart; and when this is viewed as an extension of clinical documentation, the challenges can be minimized.
4 Steps to Facilitating a POS Scanning Model
1. Partner With Clinical Leadership. Since the goal of HIMSS Stage 7 is to improve patient care through true sharing and use of patient data, creating a truly paperless stage 7 hospitalrequires the support of your clinical leadership team. Clinical leadership needs to determine that scanning is a form of clinical documentation, not an administrative task. It is then important that leadership and clinical managers collaborate to ensure full buy-in.
2. Agree on the types of documents to be scanned and who will be responsible.
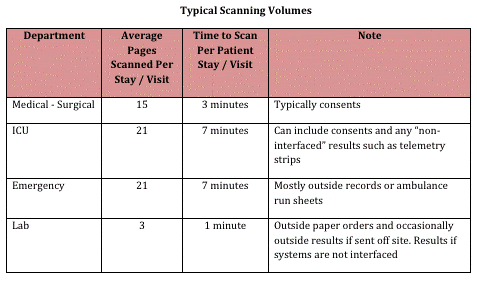
Types of documents to scan: Keep in mind that this should be a short list of no more than 10 documents (or categories of document). Agree on a list and publicize it. Remember that most documentation should be entered directly in the EHR. Going forward, scanning should be theexception. (See one hospital’s Typical Scanning Volumes chart below.)
Responsibility: Each facility will have its own staffing challenges. Our clients’ experience suggests that scanning is done by support staff and almost never by physicians and nurses. In Outpatient Ancillary departments, the front desk can scan orders and other documents as a step in the registration process. Thereafter, you may have to assign specific staff members to oversee the process.
3. Use Technology to Make It Easy. One key to obtaining buy-in from Clinical Leadership is the extent to which you make the process intuitive, easy to use and fast. At a recent implementation, we identified which forms each department would scan, defined document types and created “shortcut” buttons in the scanning interface. As a result, for a document with a patient identifier (bar code, label, etc.), the person scanning only had to select the short cut button (e.g. “consent”) which identified what they were scanning. That single step sent the document to the right patient chart and location for easy and fast record retrieval.
Although most scanning will create an image of the document, technology also exists to read and identify specific discreet data within the forms. This can have huge positive implications for assessing quality outcomes and utilizing data.
4. Partner with Health Information Management (HIM) department. HIM should own the master list of documents to scan by department. The list will include documents that must be in the patient’s record, and “miscellaneous” documents that should not be scanned. Instead of managing paper charts or scanning post discharge – HIM can complete Quality Reviews with easy access to all the data they need. Since HIM still “owns” the chart, they will be reviewing and validating scanned items and making sure they have gone to the right patient and are designated as the right document type. With streamlined and centralized work queues for document review, these tasks can often be completed in less time than it took to manage paper charts.
Conclusion
The day of the paper chart is coming to an end. Of course there are many planning considerations required to achieve success, yet it is possible to truly go paperless with a well-planned model that matches your staffing and patient care needs. Using the latest technology and collaborating with clinical teams can minimize the pain and ensure that patient care — the end goal for Stage 7 — is improved by having all clinical information in one electronic record as soon as possible for the care team.
Josh Nathan joined Freed Associates in 2012. Josh has significant project management experience in the implementation of ambulatory and inpatient electronic health record systems.


