Health Plans and New Interoperability Rules: Get Going Now.
The deadline for payers to comply with new interoperability rules is looming. Look past the technical aspects, focus on four key areas, and use compliance as a catalyst for deepening your patient relationships.

If you’re running a health plan, July 1, 2021, is closer than you think. That is the government’s deadline for putting mechanisms in place that will give your members direct access to their health information using common consumer technologies such as a smartphone.
The new rules apply to both providers and payers, but the challenge for payers is especially steep. Providers have had years of experience working through meaningful use requirements.
As a result, they already have a fundamental understanding of how to provide interoperable access from other systems to their data. Payers have some catching up to do — and fast.
In this article, Freed Associates will cover the pending interoperability requirements for health plans and suggest four smart interoperability moves to master now. But first, here’s why getting interoperability right is so important.
The Biggest Mistake Health Plans Can Make
Interoperability has been discussed and on the horizon for several years. Some health plans have been lulled into thinking it’s primarily a compliance and technical implementation issue.
It’s much more than that. The new rules redefine the way members and consumers interact with your health plan. How well you implement interoperability will have a significant future impact on your relationships with them. Our goal here is not just to help you comply with the new rules. It’s to help you determine the best ways to manage and share your data, and serve up optimal experiences to your members.
Interoperability Deadlines Looming
The intent of the new rules is this: to allow members and patients to gain secure access to their health records from both providers and payers, related to any providers that they’ve seen, anytime, and access that data from anywhere. The new rules were released this past spring by the Office of the National Coordinator (ONC) for Healthcare IT and the Centers for Medicare & Medicaid Services (CMS).
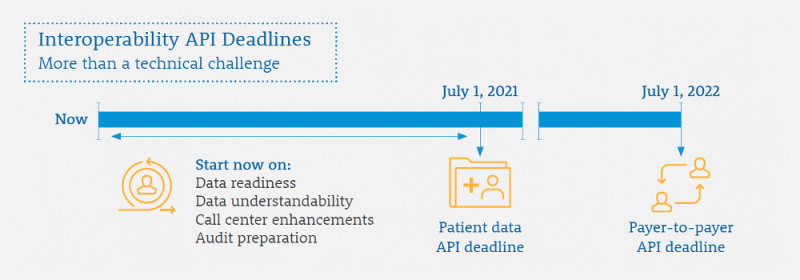
Payers Need to Put in Place Several Measures Related to Enabling Interoperability:
Make application programming interfaces (APIs) available to third-party applications. These must be in place by July 1, 2021. The APIs will allow software developers to create applications that members can use to access their plan data. You must make available access to:
- Encounter and claims information, including cost
- Specific clinical information
- Plan formulary data
- A companion provider directory API
The latter API will make your provider and pharmacy directory information publicly available so that members can find providers based on their care, treatment and care coordination interests.
Enable payer-data exchange. The next big hurdle awaiting comes around Jan. 1, 2022. By then, you need to enable payer-to-payer data exchange based on the data classes outlined in the United States Core Data for Interoperability (USCDI). This will allow consumers to more effectively transfer their data as they inevitably shift from payer to payer over the years.
Provide member education around interoperability, particularly around privacy and security.
Internally, all of this work will mean significant new or revised operational processes to support these changes. Examples include revised call scripts for handling inbound member calls, and enhanced technical acumen within the call center to assist members using a variety of third-party apps to access your plan’s new APIs.
Four Items to Focus on Now
Master your acumen around these four key interoperability moves:
- Ensure data readiness. The patient access API requires that you make a range of data accessible to your members, such as encounters, claims and clinical data, that’s within USCDI for services dating back to Jan. 1, 2016. USCDI information may have unique challenges, as it could be embedded within PDFs or images, with data coming from external providers used to adjudicate claims. Start your data analysis right away to understand where this required data resides in your source systems. Also, quickly identify whether support is needed from key vendors, such as pharmacy benefit managers, as they’ll undoubtedly receive the same requests from multiple plans.
- Improve data understandability. Claims and encounter data is not easily understood by typical plan members. Rather than mistakenly assuming that members will eventually understand this data, take proactive steps now to ensure the data is “translated” into terminology that your members can easily understand. For example, RxNorm provides normalized names for clinical drugs and links its names to many of the drug vocabularies commonly used in pharmacy management and drug interaction software.
- Enhance call center capabilities. Consider how and where to supplement your call center capabilities to ensure center personnel are prepared to address a wave of member questions regarding interoperability. For example, consider the high likelihood of members encountering difficulties accessing your data using a variety of third-party apps, then calling your call center for assistance. Will your personnel be able to effectively talk through these issues with your members? Directing members with app-related data access issues to the app maker for help will likely not be met with acclaim from members.
- Prepare for audits. The new interoperability rules are allowing plans (and providers) to gradually and gently ramp up and comply with the new standards. In the not-too-distant future, though, plans can expect to be audited on their rule compliance. You should be preparing both technically and operationally on how you will respond to complaints and audits, such as identifying what information to capture to support any inquiries.
Step Up — and Step Out in Front
Interoperability promises to provide members and patients with unprecedented access to their personal health care information. Step up and handle interoperability upgrades and changes as not just a compliance requirement but as an opportunity to better serve your members. Health plans that do so will distinguish themselves in the marketplace, and are more likely to enjoy long-term reputational and financial benefits from their efforts.
Link to Published Article (may require registration)
https://www.managedhealthcareconnect.com/content/four-steps-health-plans-can-take-advance-interoperability-improve-member-relationships


